Seeing a lab report with “uric acid” highlighted can be confusing. High uric acid is linked to gout and kidney stones, but a number by itself doesn’t tell the whole story. Below I explain what common results mean, why levels change, and practical steps you can take today to lower uric acid safely.
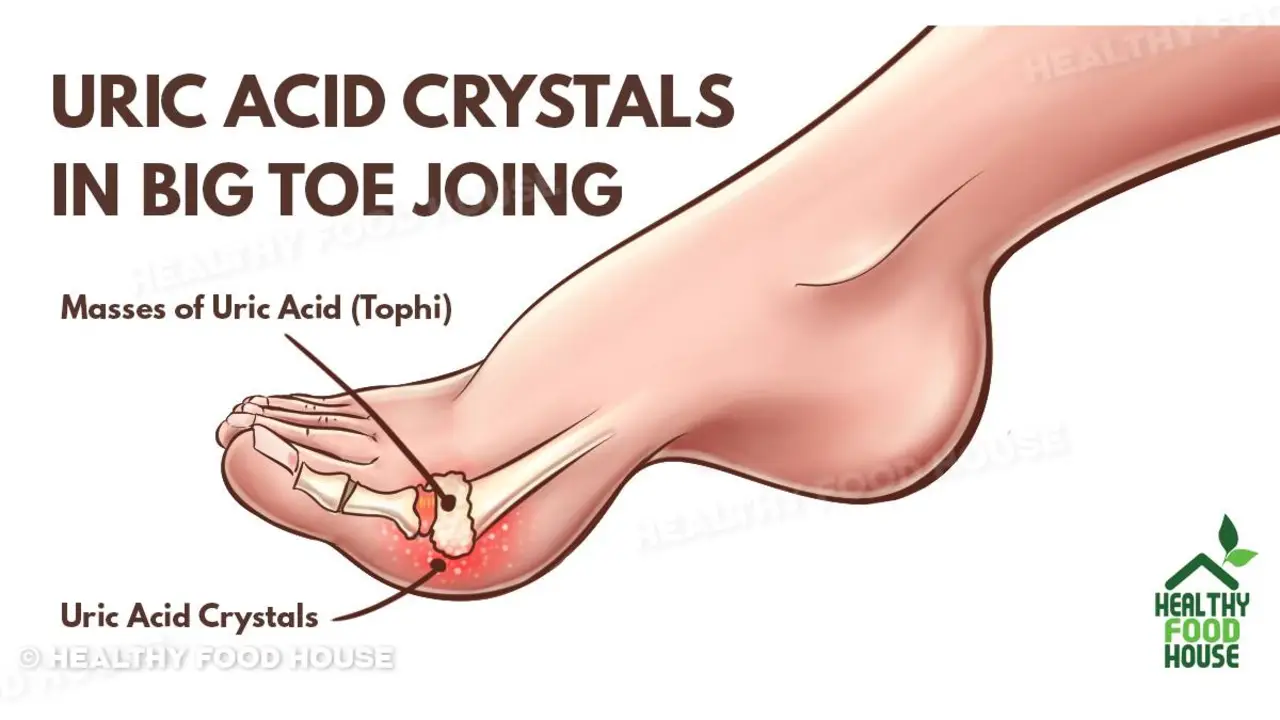
Normal blood uric acid typically sits around 3–7 mg/dL for men and 2–6 mg/dL for women. Labs vary, so check your lab’s reference range. Levels above that range are called hyperuricemia. Many people have high uric acid with no symptoms—this is called asymptomatic hyperuricemia. Symptoms to watch for: sudden joint pain and swelling (often the big toe), repeated kidney stones, or frequent joint inflammation. Causes include high-purine diet, alcohol (especially beer), sugary drinks with fructose, certain meds (like thiazide diuretics), reduced kidney function, rapid weight gain or loss, and genetic factors.
Change your plate first. Cut back on organ meats, red meat, anchovies, sardines, mussels, and other high-purine seafood. Swap sugary sodas and fruit juices for water. Even fruit juice high in fructose can raise uric acid. Choose low-fat dairy (milk, yogurt) — studies show dairy can help lower levels. Eat more vegetables, whole grains, and cherries or cherry juice occasionally; cherries have shown modest benefit for gout flare prevention.
Drink water. Aim for steady hydration to help kidneys flush uric acid; 8–12 cups a day is a reasonable starting point unless your doctor gives other advice. Lose weight slowly if you’re overweight—rapid weight loss can temporarily raise uric acid. Move more: regular moderate exercise helps insulin sensitivity and long-term uric acid control.
Limit alcohol. Beer and spirits raise uric acid and the risk of gout attacks more than wine. If you drink, keep it minimal and track how your body reacts.
Check your medicines. Some blood pressure drugs and low-dose aspirin can raise uric acid. Don’t stop meds without talking to your provider—there are often alternatives or workarounds.
If lifestyle changes aren’t enough, medication can help. The common long-term options are xanthine oxidase inhibitors like allopurinol or febuxostat, which reduce uric acid production, and uricosurics like probenecid that help the kidneys remove uric acid. Your doctor will pick a drug based on your health, kidney function, and history of gout attacks. Regular follow-up labs are needed when on these drugs.
When to see a doctor right away: severe joint pain with swelling, symptoms of a kidney stone (sharp back or side pain, blood in urine), or sudden high fever with a hot, swollen joint. For ongoing high uric acid, a primary care doctor or rheumatologist can set targets and a treatment plan.
Quick checklist: check your lab’s range, cut high-purine foods and sugary drinks, hydrate, limit alcohol, lose weight slowly, review meds with your doctor, and get medical treatment if you have gout attacks or stones. Small, steady changes usually make the difference.
Hi there, gentlemen! In today's blog post, we're going to tackle some of the most common myths and misconceptions surrounding high uric acid levels and gout. I bet you've heard many of them before, but rest assured, our aim is to debunk these myths and arm you with the facts. Let's navigate this journey together, separating fact from fiction when it comes to your health.
Compare Natrise (tolvaptan) with safer, cheaper alternatives for treating hyponatremia. Learn when fluid restriction, urea, or demeclocycline may be better options - and why Natrise isn't always the right choice.
Navigating exercise with an overactive bladder can be tricky, but you don’t have to give up being active. This article breaks down how movement affects OAB, which types of workouts actually help, and what to avoid if you want to prevent leaks or accidents. Get practical tips on managing symptoms before, during, and after exercise, plus advice for building confidence when trying new routines. Say goodbye to embarrassment and uncertainty—everything here is designed for people ready to be active on their terms.
Fluticasone nasal spray and oral steroids both reduce inflammation, but they work very differently. Learn why nasal spray is safer for allergies and when oral steroids are actually needed.
Switching health plans? Your generic drug coverage can change drastically - and cost you thousands. Learn how to check formularies, understand tiers, and avoid surprise prescription costs.
Affirmative consent laws don't apply to medical decisions. Learn how real patient permission works through informed consent and substituted judgment when you can't speak for yourself.