High eye pressure (also called ocular hypertension) means the fluid pressure inside the eye is above the typical range. Doctors usually measure intraocular pressure (IOP) in millimeters of mercury (mmHg); roughly 10–21 mmHg is considered normal for many people. High readings don’t always mean you have glaucoma, but they raise the risk of optic nerve damage that can steal your vision over time.
Eye pressure is checked with a tonometer. The common quick test is a puff of air (non-contact tonometry) or a gentle probe after numbing drops (applanation tonometry). Your eye doctor may also do pachymetry (measures cornea thickness), OCT imaging (takes photos of the optic nerve and retina), and visual field testing (checks side vision). These extra tests tell the doctor whether elevated pressure is already affecting the optic nerve or vision.
Why cornea thickness matters: a thicker or thinner cornea can make the pressure reading look higher or lower than it really is. That’s why doctors combine tests rather than rely on one number.
Treatment depends on your risk and test results. If your optic nerve and fields look normal, your doctor might suggest monitoring with regular checkups. If they see nerve damage or a high risk of damage, treatment usually starts with eye drops. Common classes of drops include prostaglandin analogs, beta blockers, alpha agonists, and carbonic anhydrase inhibitors. Each works differently to lower pressure; your doctor will pick what fits your health and lifestyle.
If drops don’t work well enough, laser trabeculoplasty is a common next step. It helps improve fluid outflow in many patients. For more advanced or resistant cases, surgical options such as trabeculectomy or drainage devices may be recommended. Your eye surgeon will explain benefits and risks so you can choose with confidence.
Everyday habits that help: keep follow-up appointments, take prescribed drops exactly as directed, and tell your doctor about other medicines you take. Moderate aerobic exercise can help eye health for many people. Avoid smoking and talk with your doctor about limiting high caffeine doses if that’s a concern. If you notice sudden eye pain, nausea, blurry vision, or halos around lights, seek care immediately—those can be signs of an acute angle-closure emergency.
Tracking is useful: save IOP numbers and test results, note when you start or stop a drop, and bring this record to visits. If you’re unsure about a diagnosis or plan, a second opinion from a glaucoma specialist is reasonable. Regular eye checks—intervals your doctor sets—are the best way to protect vision when pressure is high.
High eye pressure is manageable in most cases. With the right tests, treatment, and follow-up you can reduce risk and keep your eyesight strong.
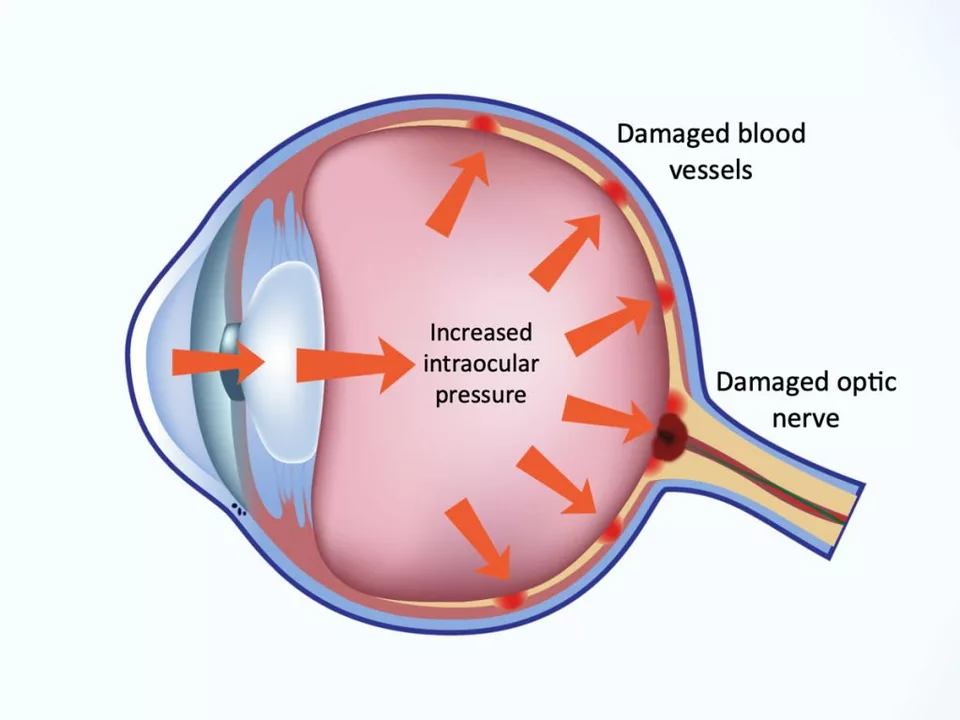
In a recent blog post, I discussed the link between high eye pressure and glaucoma, a potentially blinding eye disease. I learned that high eye pressure, also known as ocular hypertension, can damage the optic nerve and lead to glaucoma. It's important to have regular eye exams to detect any changes in eye pressure early on. While not everyone with high eye pressure will develop glaucoma, it is still a significant risk factor. Therefore, it's essential to be proactive in managing eye pressure and maintaining overall eye health.
Statins and ALS: No proven link exists. Latest research shows long-term statin use may reduce ALS risk, while early symptoms often cause mistaken fear. Don't stop statins without medical advice.
Choline salicylate and lignocaine are transforming geriatric pain management by offering effective, non-opioid relief with minimal systemic risk. Ideal for arthritis and muscle pain in seniors, this topical combo avoids stomach and kidney side effects common with oral meds.
Learn how to safely carry and refill medications abroad, avoid legal trouble, and get local prescriptions when traveling. Essential tips for travelers with chronic conditions, mental health meds, or pain management needs.
Get the facts on Biltricide (Praziquantel): its uses, how it works, side effects, safety tips, and practical advice for treating tapeworms, liver flukes, and schistosomiasis.
Ankylosing spondylitis causes chronic spine inflammation and can lead to fusion if untreated. Learn how medication, daily exercise, and lifestyle changes can preserve mobility and prevent long-term damage.